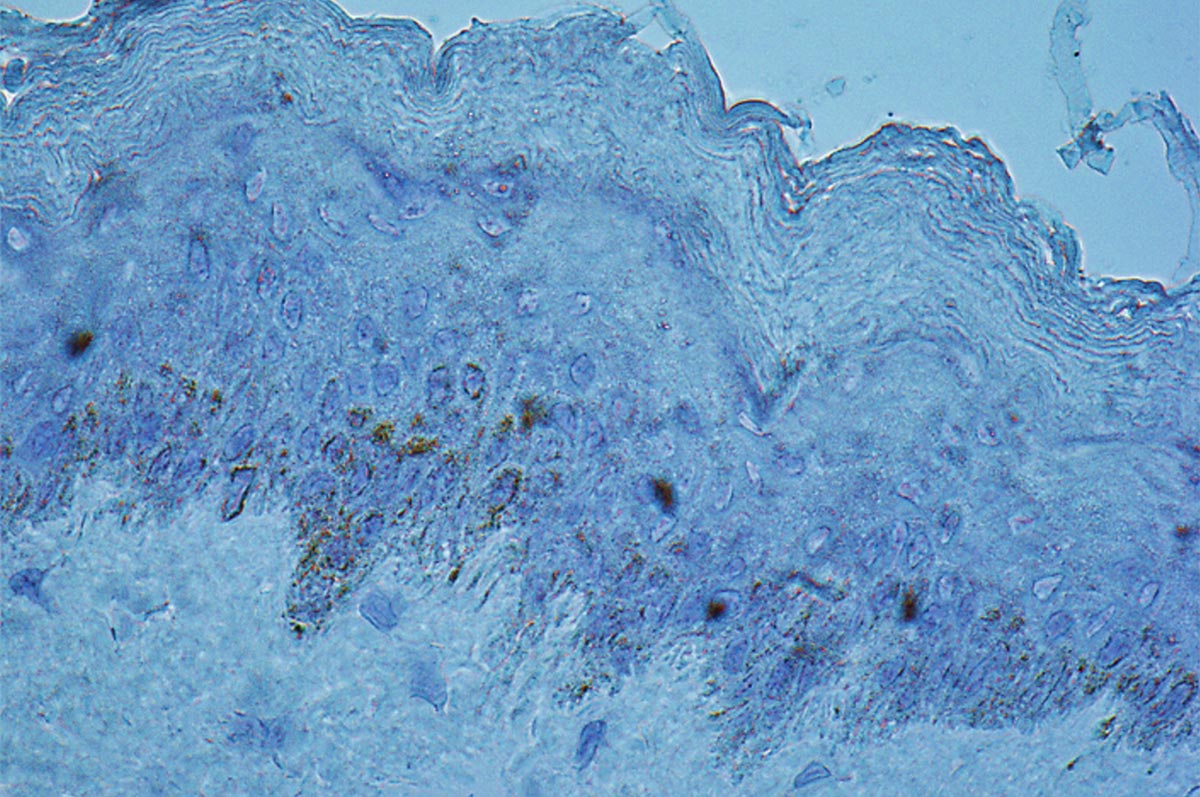
Context and Challenges
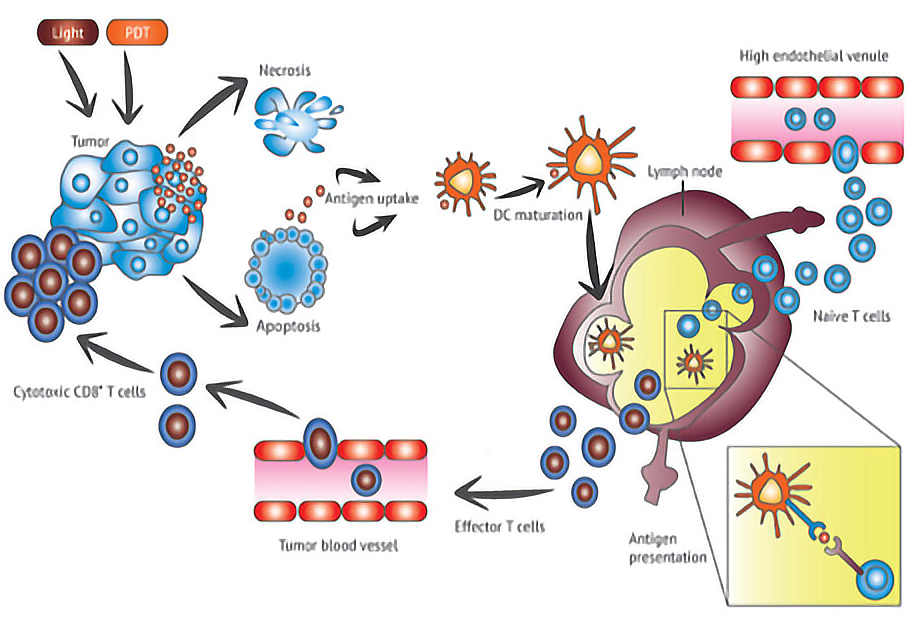
The use of PDT in the field of oncology has already proved its worth and has been the subject of growing interest in recent years. Today, there is a real rational for thinking that PDT could impact the immune response, in favour of immunoactivation. This property would be a considerable asset in the management of cancers if we take into account the success of certain anti-tumour immunotherapies (anti-PD1, PDL1, CTLA-4, etc.), particularly in the last 3 years.
Within the OncoThAI unit, the ImmunoPDT team led by Pr Nadira DELHEM works in close association with the PhysicoPDT team led by Dr Anne-Sophie Dewalle, and in collaboration with clinicians from the Lille CHRU and the Centre Oscar Lambret. The five major projects developed within the team aim to better understand the impact of PDT on the immune response by evaluating more specifically the mechanisms involved in the immuno-modulation of the immune system by PDT.
The realization of these projects requires a double expertise, that acquired historically by the team "Immunoregulation of Viro-Induced Cancers" led by Pr Nadira Delhem, in the fields of immunosurveillance and cancers' immunotherapy, and that acquired by "Physico PDT" team in the field of lasers and photodynamic therapy. The synergy of these skills will enable us to understand the role of PDT in immune regulation upstream, in order to propose innovative protocols for the treatment of cancers.
Objectives
The INSERM U1189 unit, in collaboration with the clinical departments of Gynecology, Digestive Transplantation, Neurosurgery, Dermatology and Pneumology of the Lille CHRU, has started five ambitious projects which aimed to evaluate, in parallel, the efficacy of PDT as an anti-tumor treatment and the impact of PDT on the regulation of the immune response. This translational work is taking place in two areas: clinical and research. In terms of research, the immunoPDT team proposes to develop fundamental projects further upstream of translational research, aiming to understand at the biological and molecular level, the impact of PDT on both tumour cells and immune cells [IM-PRODYNOV (ovarian carcinosis) and HEPATOCAR (hepatocarcinoma) projects].
This work is being carried out in two areas: clinical and research. In terms of research, the immunoPDT team proposes to develop fundamental projects further upstream of translational research, aiming to understand at the biological and molecular level, the impact of PDT on both tumour cells and immune cells [IM-PRODYNOV (ovarian carcinosis) and HEPATOCAR (hepatocarcinoma) projects].
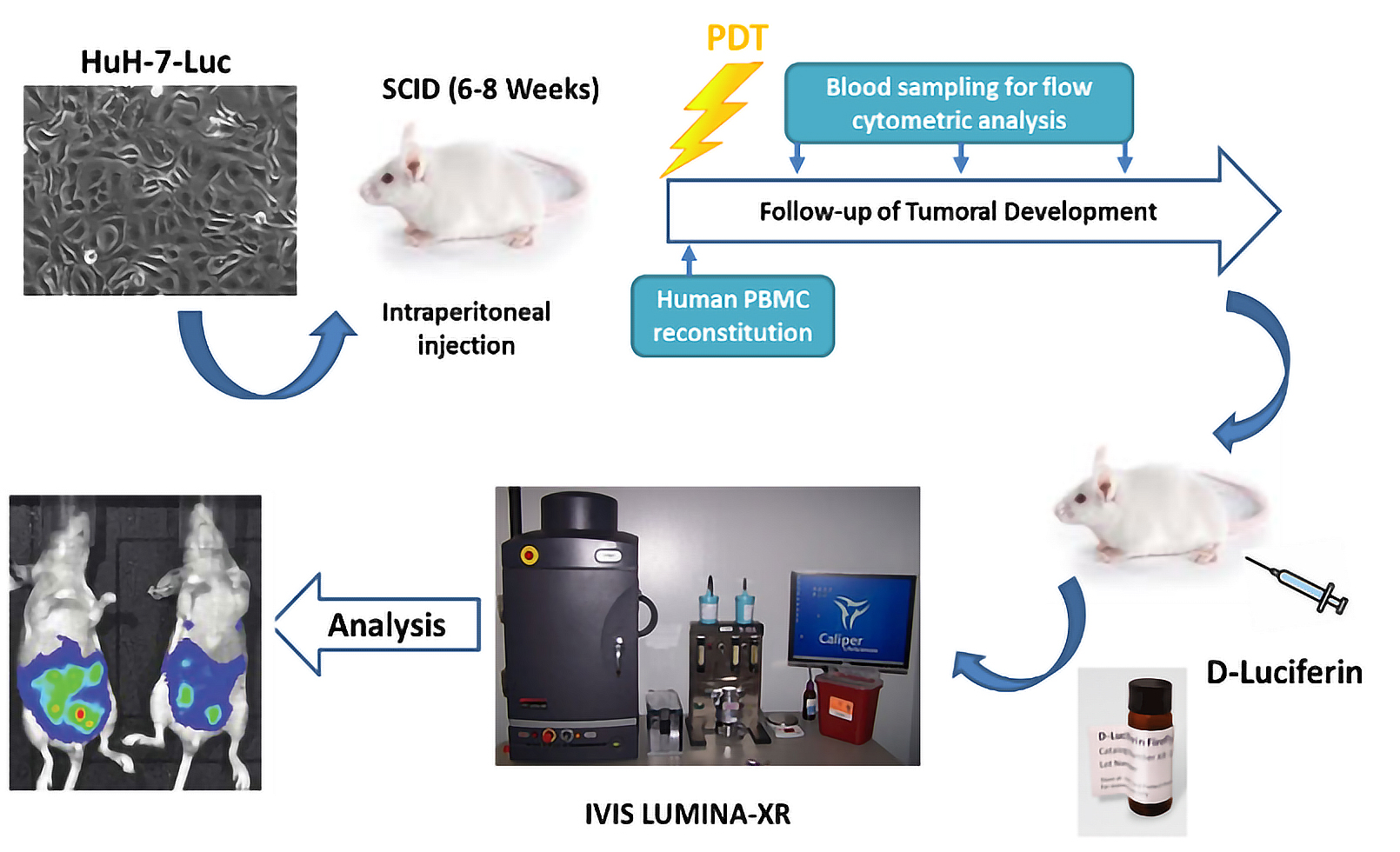
In addition, the ImmunoPDT team has developed high-performance methodological tools and techniques for the in vivo evaluation of new anti-tumor therapeutic strategies.
In particular, the team has developed innovative "custom" humanized mouse models that combine xeno-transplantation of human tumors expressing luciferase with reconstitution with a human immune system.

These models, which are easily exploitable in small animal imaging, make it possible to develop anti-tumor strategies in a context very close to human physiopathology.
In order to evaluate in these in vivo models the efficacy of PDT and its impact on a human immune system, unit U1189 has developed innovative devices for in vivo illumination of mice.
At the clinical level, the ImmunoPDT team is developing more translational research projects aimed at characterizing the effects of PDT, combined with surgery or immunotherapy, on the phenotype and activation of immune cells (immunomonitoring) and on the regulation of the immune response (regulatory T lymphocytes, tolerogenic DC, tumor exosomes, etc.). All of these studies are carried out using samples from patients included in clinical trials or ancillary studies [IM-INDYGO (glioblastoma), IMCUTALA (melanoma) and IMPALA (mesothelioma) projects].
Where are we with our research?
Thanks to the financial support of SATT Nord de France and SATT Grand-Est, a patent on a new photosensitizer (PS), specifically targeting peritoneal ovarian carcinosis, has been filed. The photosensitizer (PS-FOL) presented here is the product of an original synthesis carried out by the team of the Reaction and Process Engineering Laboratory (LRGP - UMR 7274 CNRS - University of Lorraine). The objective of this synthesis is to associate the PS with an addressing molecule (folic acid) targeting FR with a strong affinity. We cannot further detail the nature of this compound for confidentiality reasons.
Our main objective was to evaluate PDT in this indication and its impact on the immune response. Initial in vitro results showed an excellent efficacy of PDT on human ovarian carcinoma cell lines.
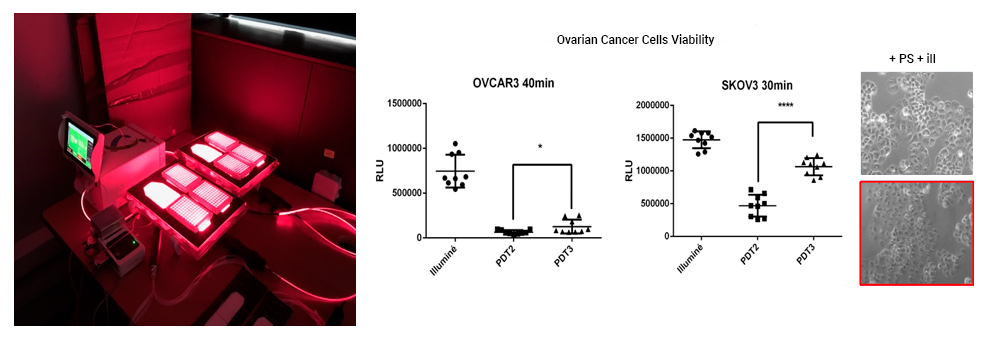
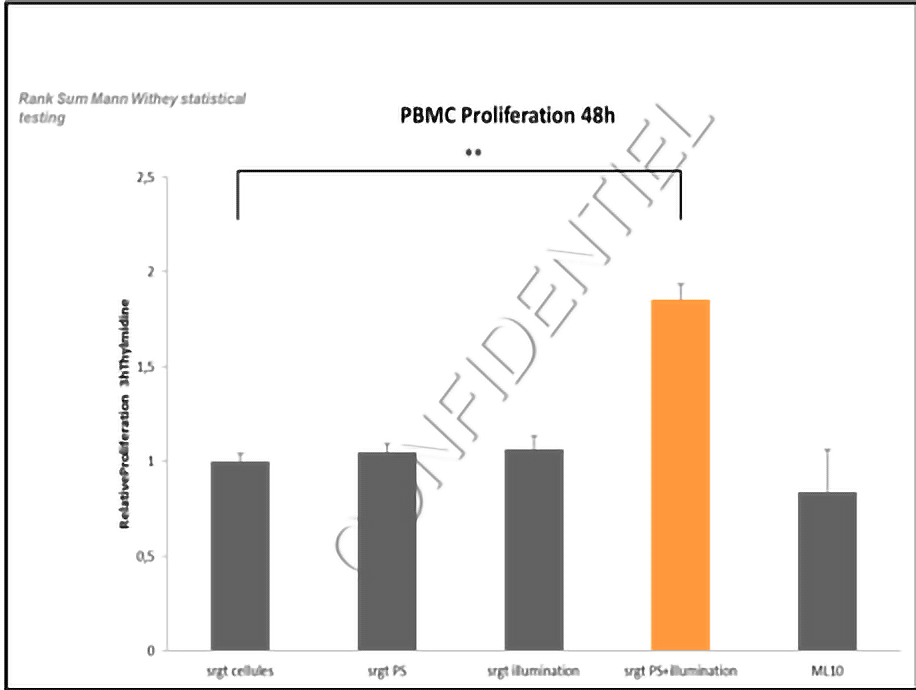
Furthermore, PDT also has a beneficial effect on the immune system. The observed results show that tumour cells subjected to PDT produce immunostimulatory factors by inducing an increase in the proliferation of human immune cells.
PDT also induces a decrease in the production of pro-inflammatory cytokines by tumour cells and an increase in cytokines that are favourable to the survival, proliferation and activation of immune cells, mainly for CD4+ T and CD8+ T lymphocytes, such as the cytokines IL2, IFN-gamma.
In the context of hepatocellular carcinoma (HCC), we were able to obtain very promising initial results thanks to international thesis funding. The main objective of this study is to understand, in the context of HCC, the direct and indirect effects of 5-Aminolevulinic Acid (5-ALA)-mediated HCC.
In this context, hepatic cancer cell lines have been used in a first step: HuH7 (overexpressing p53), Hep3B (partial deletion of p53) and HepG2 (expressing wild p53) and in a second step primary HCC cells from surgical excision will be used.
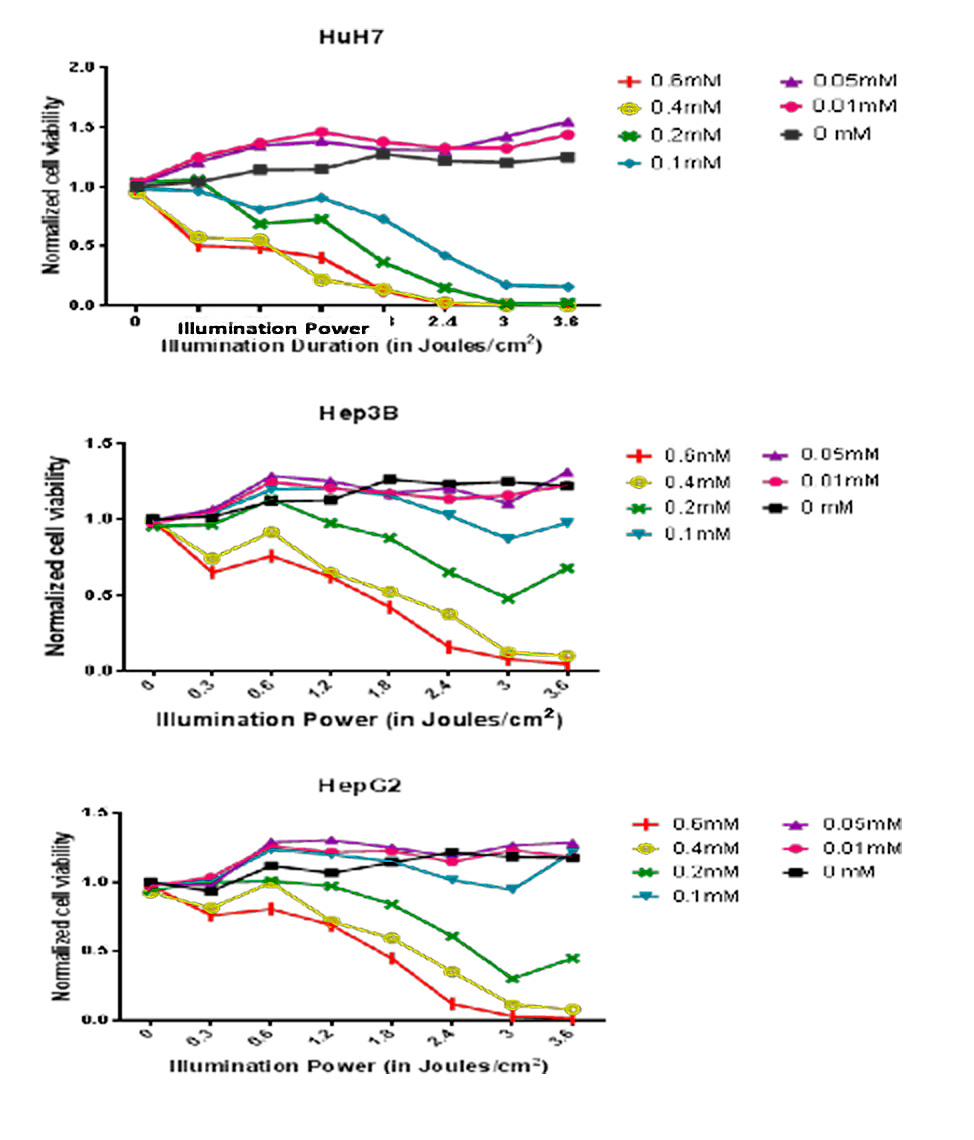
Our preliminary results showed that PDT can be effective against the three different HCC cell lines because they express the key enzymes responsible for the conversion of the pro-drug 5-ALA into Porphyrin IX (PpIX), the final PS.
Thus, PDT treatment with 5-ALA in these cell lines induces cell death that is dependent on the dose of 5-ALA and the duration of illumination.
Interestingly, we also observed that these three cell lines respond variably to 5-ALA PDT in a pattern that appears to be related to the p53 expression profile.
Moreover, thanks to a very close collaboration network with clinicians from the CHRU of Lille and the Centre Oscar Lambret and thanks to the logistic and financial support of industrials (Novartis, BMS and MSD), we have initiated two new projects in the framework of Melanoma and Mesothelium.
Immunotherapies, such as anti-PD-1 antibodies, have emerged in recent years as a major therapeutic tool in many cancers. Thus, the advantages provided by both immunotherapy and PDT have led us to propose a combination of the two treatments in order to improve the local anti-tumor effect in patients with melanoma with skin metastases, or with mesothelium.
Based on a rational synergistic effect of PDT and immune checkpoint inhibitors, we hope to induce a strong anti-tumor immune response, in the absence of cumulative toxicities, leading to a better outcome for these patients.